Complex Trauma
AKA Developmental Trauma
Many times kids are diagnosed with ADHD, bipolar or having PTSD (posttraumatic stress disorder) but it may be more than that. While a child may seem to be inattentive and have ADHD, you know as a parent that it doesn’t quite explain all of the child’s problems. It may be complex trauma.
To learn how we can help, contact us or call 224-208-5228
What is complex trauma?
The National Child Traumatic Stress Network defines complex trauma as a term that describes both children’s exposure to multiple traumatic events, often of an invasive, interpersonal nature, and the wide-ranging, long-term impact of this exposure. These events are severe and pervasive, such as abuse or profound neglect. They usually begin early in life and can disrupt many aspects of the child’s development and the very formation of a self. Since they often occur in the context of the child’s relationship with a caregiver, they interfere with the child’s ability to form a secure attachment bond. Many aspects of a child’s healthy physical and mental development rely on this primary source of safety and stability.
Sometimes after a child experiences a negative event, their development freezes. This can start to change the trajectory of their life. Now the consequences of the negative event are further reaching, thus the name developmental trauma or complex trauma.
More on complex trauma here.
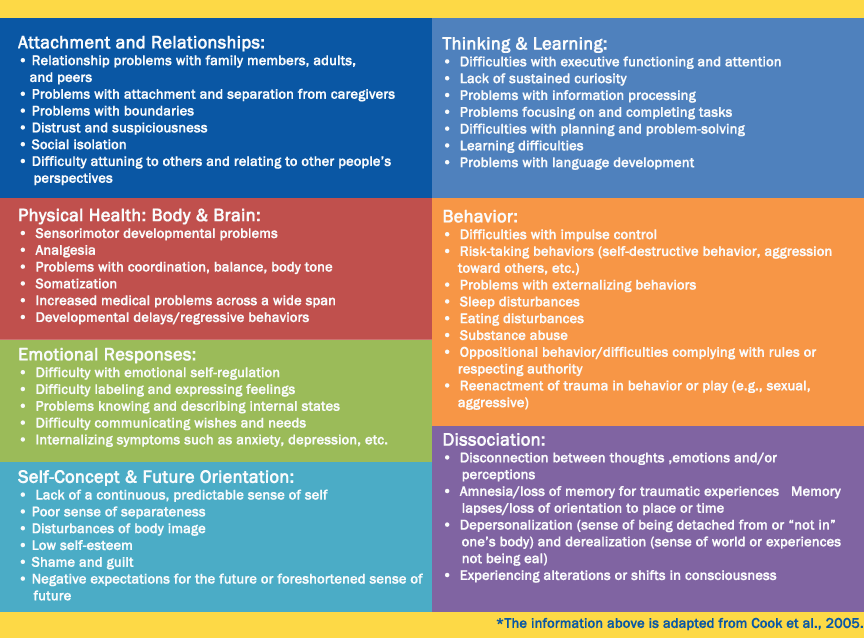
More on the effects of complex trauma here.

Might my child have complex trauma?
A brief complex trauma assessment
The following assessment is taken from NCTSN.org (a national website of collaboration to help treat trauma in the US)
Accurate assessment is important because it helps clinicians to choose the best treatment possible. Children and adolescents with complex trauma may have a wide range of symptoms. Different children can have different combinations of symptoms, and these symptoms may change over time. How a child reacts depends on age, experiences, personality, strengths, and individual vulnerabilities.
There currently is no official diagnosis that captures the full range of complex trauma symptoms. However, through a comprehensive assessment, informed and experienced mental health professionals can help determine if your child’s problems are related to complex trauma. Children with complex trauma sometimes carry multiple diagnoses (for example, bipolar disorder, attention deficit hyperactivity disorder, post-traumatic stress disorder, and so on) for which they may be prescribed several different medications. This may happen when the professionals making the diagnoses have not fully taken into account the impact of the child’s trauma history. This can lead to a child’s receiving improper diagnoses or treatment.
Please read the statements below. If you answer yes to two or more, you may want to consider referring your child for a complete assessment for complex trauma. The survey below is a tool to help you decide when you need to seek professional help.
My child has been exposed to many potentially traumatic experiences.
My child has difficulty controlling emotions and easily can become sad, angry, or scared.
My child has trouble controlling behaviors.
My child often exhibits significant changes in activity level, appearing overactive or agitated sometimes and then calmer, or even quite slowed down at other times.
My child has trouble remembering, concentrating, and/or focusing. He/she sometimes appears “spacey.”
My child has problems with eating, sleeping, and/or complains about physical symptoms even though doctors find nothing physically wrong to explain these symptoms.
My child has difficulties in forming and sustaining relationships with other children and adults.
My child seems to need and seek out more stimulation than other children and/or can be easily distracted by noises, sounds, movements, and other changes in the environment.
My child has many mental health diagnoses but none of them quite seem to explain his/her problems.
My child is taking medication (or many medications) for these diagnoses but the medicines are not helping.